Knee Arthritis
Arthritis is a general term that relates to cartilage loss and/or dysfunction within a joint. The most common form of knee arthritis is osteoarthritis, commonly referred to as “degenerative” or “wear and tear arthritis.”
What Causes Knee Arthritis?
Knee arthritis is caused by a combination of genetics, activity level, medical comorbidities, and prior injuries or surgeries. Other causes of arthritis include: post-traumatic (prior injury), inflammatory (such as rheumatoid or lupus), infectious, and osteonecrosis (loss of blood supply to the bone).
Knee Arthritis Symptoms
The most common symptoms of knee arthritis include:
- Pain with activity
- Pain that is achy, dull or sharp
- Stiffness and swelling in the knee
- Mechanical popping or grinding
- Maligned knees (bow-legged or knock-kneed)
Knee arthritis symptoms typically worsen over time, and pain can be present even at rest or at night. Everyday activities such as walking, going up and down stairs, squatting, pivoting and kneeling can become harder as the condition progresses.
Symptoms can vary in severity and may come on suddenly or be persistent. For some patients, these symptoms slowly worsen over a long period of time. For other patients, the knee functions very well until it eventually and suddenly “flairs flares up” and becomes very symptomatic over a short period of time.
How is Knee Arthritis Diagnosed?
Diagnosis is based on history, physical exam, and imaging studies. Patients frequently complain of symptoms as discussed above. On exam, patients often limp, the leg may be malaligned (displacement of bones out of line in relation to joints), the knee is often swollen, with decreased range of motion, tenderness, and palpable grinding with range of motion.
The most common imaging tests to diagnose knee arthritis include:
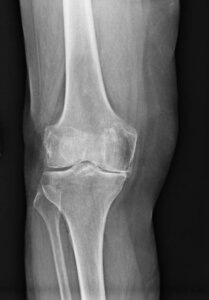
- X-rays: X-rays show us the condition of the bone. On x-rays, we look for loss of joint space (which suggests that the cartilage and menisci are worn out), bone spurs, and cysts within the bone.
- MRIs: MRIs show us the condition of the soft tissues including the cartilage, ligaments, and meniscus. MRIs are not typically needed for routine evaluation of knee arthritis. In severe cases, x-rays are more than sufficient. MRIs are most beneficial when x-rays show only mild degenerative changes where the pain patients are having is more than we would expect based on the severity of the x-rays.
To learn more about how we diagnose through imaging, and our imaging capabilities, check out our X-Ray & Imaging service.
Knee Arthritis Treatment
We always recommend starting with nonoperative treatment first. While it is not possible to regrow cartilage or to make the knee totally normal again, there are options to relieve pain. While treatment plans are individualized to specific patient situations, non-surgical options for knee arthritis include:
- Injections
- Anti-inflammatory
- Physical therapy
- Activity modification
Knee Injections
In general, there are two categories of injections we routinely use: steroid injections and hyaluronic acid injections. Both medications act to decrease inflammation in the knee to reduce pain and swelling. There are pros and cons to each type of injection, which you should discuss with your surgeon.
Is it Possible to Regrow Cartilage? What about Stem Cells?
There are treatment options available such as PRP (platelet-rich plasma) or stem cell injections. These procedures are not covered by insurance for treatment of arthritis because there is no data or research that shows them to be beneficial. Hopefully we will be able to regrow cartilage in the future, but there is currently no technology that makes this possible inside of an arthritic joint. Because there is no scientific evidence to support the benefits of these injections, we do not currently offer them for the treatment of knee arthritis.
What are the Surgical Options for Knee Arthritis?
- Arthroscopy: Sometimes people will refer to having an arthroscopic procedure performed to “clean out” the arthritis from the knee. This is generally a misnomer. Knee arthroscopy performed in patients with arthritis may be indicated in some situations, but this procedure can often result in little improvement and sometimes worsening of symptoms.
- Osteotomy: This procedure involves cutting and repositioning of the bone. These procedures are mostly historical. In today’s practice, osteotomies are generally reserved for very young patients who do not wish to undergo knee replacement, and have arthritis or cartilage damage limited to only one compartment of the knee.
- Partial Knee Replacement: Partial knee replacement, also known as unicompartmental knee replacement, involves an incision in the knee and a removal of the arthritic surfaces from only the areas of the knee are being replaced.
- Total Knee Replacement: Total knee replacement involves removing the arthritic surfaces of the bone and replacing them with metal or ceramic caps.
Request an Appointment with a Knee Physicians
If you are experiencing knee pain or believe you have knee arthritis, contact us to schedule a consultation. Our Joint Replacement Team has extensive experience in treating knee arthritis from nonoperative treatments to minimally invasive total knee replacements.
